Ulnar Impaction Syndrome Treatment in Raleigh, NC
What is Ulnar Impaction Syndrome?
Ulnar impaction syndrome (UIS), also known as ulnar abutment syndrome or ulnocarpal impaction syndrome, is a degenerative condition affecting the ulnar (pinky finger) side of the wrist. This condition results from excessive load transfer across the triangular fibrocartilage complex (TFCC) and the ulnocarpal joints, leading to characteristic degenerative changes and chronic wrist pain.
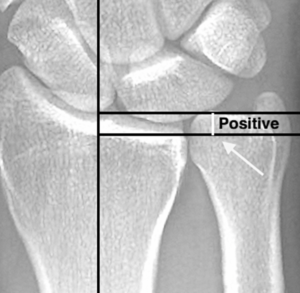
The syndrome occurs most commonly in patients with positive ulnar variance—a condition where the ulna bone is longer than the radius bone at the wrist joint. This anatomical variation causes increased pressure and mechanical stress on the ulnar side of the wrist during gripping and forearm rotation activities.
Causes and Risk Factors
Primary Causes
Positive Ulnar Variance: The most significant risk factor for ulnar impaction syndrome is positive ulnar variance, which can be either static (present at rest) or dynamic (occurring only during certain wrist positions or activities).This anatomical variation leads to excessive load bearing across the ulnar carpus, TFCC, and ulnar head.
Degenerative Changes: UIS is fundamentally a degenerative condition that develops over time due to repetitive stress and overload on the ulnar structures of the wrist.
Contributing Factors
– Athletic activities involving repetitive wrist loading and gripping
– Occupations requiring repetitive forearm rotation and wrist use
– Previous wrist injuries or trauma
– TFCC tears or defects
Clinical Presentation and Symptoms
Common Symptoms
Patients with ulnar impaction syndrome typically present with:
– Ulnar-sided wrist pain: The hallmark symptom, located on the pinky finger side of the wrist
– Activity-related pain: Symptoms worsen with gripping, forearm rotation, and weight-bearing activities
– Pain that persists: Unlike simple strains, the pain does not improve with rest
– Limited range of motion: Reduced wrist mobility, particularly with ulnar deviation
– Weakness: Decreased grip strength compared to the unaffected side
Physical Examination Findings
Healthcare providers use several provocative maneuvers to diagnose UIS:
– Ulnar impaction test: Pain with axial loading of the wrist in ulnar deviation
– Piano key test: Assessment of distal radioulnar joint stability
– Foveal stress test: Evaluation of TFCC integrity
Diagnostic Evaluation
Imaging Studies
Plain Radiographs: Initial imaging typically includes standard wrist X-rays to measure ulnar variance. Positive ulnar variance is the characteristic finding in ulnar impaction syndrome.
Magnetic Resonance Imaging (MRI): MRI is essential for confirming the diagnosis and evaluating associated soft tissue pathology. MRI findings in UIS include:
– TFCC tears or degeneration
– Cartilage damage (chondromalacia) of the lunate and triquetrum
– Bone marrow edema in the ulnar carpus
– Subchondral cystic changes
MRI allows earlier detection of abnormalities in the TFCC, cartilage, and bone marrow compared to plain radiographs and helps exclude other causes of ulnar-sided wrist pain.
Wrist Arthroscopy: Diagnostic arthroscopy can confirm the clinical diagnosis and facilitate appropriate surgical management when imaging findings are equivocal.
Differential Diagnosis
Ulnar-sided wrist pain has been referred to as the “black box” of the wrist due to its complex differential diagnosis.Other conditions to consider include:
– TFCC tears (without impaction)
– Lunotriquetral ligament injuries
– Ulnar styloid impaction syndrome
– Extensor carpi ulnaris tendinitis
– Distal radioulnar joint arthritis
– Pisotriquetral arthritis
Treatment Options
Conservative Management
Non-operative treatment is recommended as the initial approach for ulnar impaction syndrome.Conservative management typically includes:
Immobilization: Short arm orthosis or splinting for 6 weeks to reduce stress on the ulnocarpal joint
Physical Therapy: Formal physiotherapy program following immobilization, typically lasting 6 weeks
Activity Modification: Limiting aggravating movements and avoiding repetitive gripping and forearm rotation activities
Anti-inflammatory Medications: NSAIDs to manage pain and inflammation
Success Rates of Conservative Treatment
Studies show that approximately 59% of patients respond successfully to conservative treatment at 24-week follow-up.[6]Factors associated with treatment failure include:
– Female gender
– Longer duration of symptoms
– Higher pain scores on provocation testing
– Bone marrow edema on MRI
Surgical Treatment
When conservative management fails, surgical intervention is indicated. The two primary surgical options are:
1. Ulnar Shortening Osteotomy (USO)
This procedure involves cutting the ulnar bone and removing a segment to shorten it, thereby reducing the load across the ulnocarpal joint. The bone is then fixed with a plate and screws
Advantages:
– Addresses the underlying anatomical problem
– Effective for all degrees of positive ulnar variance
– Restores normal biomechanics
Disadvantages:
– Longer recovery time (union typically by 12 weeks)
– Higher complication rates, including hardware irritation, nonunion, and refracture
– Delayed return to work
– May require secondary surgery for plate removal
2. Arthroscopic Wafer Procedure (AWP)
This minimally invasive arthroscopic technique involves resecting 2-4mm of the distal ulnar head to decompress the ulnocarpal joint.
Advantages:
– Minimally invasive approach
– Faster recovery and earlier return to work
– Lower complication rates
– No hardware-related issues
– Single-stage procedure
Disadvantages:
– Limited amount of shortening possible
– May not be suitable for severe positive ulnar variance (>4mm)
– Requires arthroscopic expertise
Comparing Surgical Outcomes
Recent high-quality studies comparing AWP and USO have shown:
Short-term outcomes (3-6 months): AWP demonstrates superior results with better grip strength, Mayo Wrist Scores, and DASH scores, along with earlier return to work
Long-term outcomes (2-10 years): Both procedures provide excellent pain relief and functional improvement. A 10-year follow-up study showed sustained benefits with both techniques, though AWP achieved slightly better DASH scores (4.35 vs 12.7) at final follow-up
Complication rates: AWP consistently shows lower complication rates (10.5%) compared to USO (34.8%), with USO complications primarily related to hardware irritation requiring removal
Clinical equivalence: Meta-analyses confirm no significant differences in pain improvement or functional scores between the two procedures, though AWP offers advantages in recovery time and complication profile
Prognosis and Outcomes
The overall prognosis for ulnar impaction syndrome is favorable with appropriate treatment:
– Surgical intervention, when needed, is often curative
– Both AWP and USO reliably reduce pain and improve function over at least 10 years
– Patient satisfaction rates are high with both surgical approaches
– Return to sports and occupational activities is expected, though timing varies by procedure
Why Choose Dr. Chambers for Hand and Wrist Care
At Raleigh Orthopaedic Clinic, Dr. Stephen Chambers specializes in hand and upper extremity surgery. With years of expertise in treating hand and wrist injuries, including Ulnar Impaction Syndrome Treatment. Dr. Chambers provides comprehensive care—ranging from at home treatments and injections to advanced hand surgery when needed. Patients trust Dr. Chambers and his team for personalized care, effective treatment options, and excellent outcomes and describe Dr. Chambers as a caring, attentive, and skilled surgeon with excellent bedside manner. His amazing team ensures every patient feels supported and informed throughout the process.
If you are experiencing wrist pain, swelling, or difficulty with wrist movements, don’t wait for symptoms to worsen. Schedule an Appointment with Dr. Chambers today to Ulnar Impaction Syndrome Treatment. and get back to normal use of your hand . Experience the benefit of specialized hand care close to home at Raleigh Orthopaedics in Raleigh, Cary, Holly Springs, and Wake Forest, North Carolina.

