Treatment for Pediatric Elbow & Supracondylar Fracture in Raleigh, NC
Overview
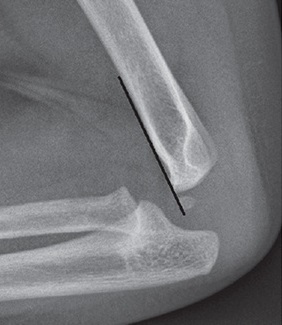
Supracondylar fractures of the humerus are the most common elbow fractures in children, accounting for more than half of all pediatric elbow injuries. These fractures typically occur in children aged 5-7 years, most commonly from a fall onto an outstretched hand with the elbow in extension. Treatment decisions are guided by the Gartland classification system, which categorizes fractures based on displacement and helps determine whether conservative or surgical management is appropriate.
Treatment Options
Non-Operative Management
Indications:
– Non-displaced or minimally displaced
– Selected Type IIA fractures with isolated extension deformity and no rotational or coronal plane malalignment
Method:
– Long-arm cast immobilization with elbow flexed at 90 degrees
– Close radiographic follow-up at regular intervals
– Duration: 3-4 weeks typically
Outcomes:
Recent evidence suggests that approximately 90% of Type IIA fractures can be successfully treated nonoperatively with close monitoring. However, nonoperative management carries a treatment failure rate of 8.9-20.6% requiring subsequent surgery.
Operative Management
Indications:
– Completely displaced
– Type II fractures with rotational deformity, varus/valgus malalignment, or shaft-condylar angle 30 degrees
– Neurovascular compromise requiring immediate intervention
Preferred Technique:
Closed reduction and percutaneous pinning (CRPP) is the gold standard for displaced supracondylar fractures. The American Academy of Orthopaedic Surgeons provides a moderate strength recommendation for closed reduction with pin fixation for displaced (Type II and III) pediatric supracondylar fractures.
Emergency Surgery Required:
– “White hand” without palpable pulse (vascular compromise)
– Compartment syndrome
– Open fractures
Pin Removal
K-wires should be removed 3-6 weeks after surgery once fracture consolidation is confirmed on radiographs.
Management of Complications
Neurovascular Injuries
Nerve Injuries:
– Prevalence: 5-19% of supracondylar fractures
– Most are neurapraxias that resolve with conservative management
– Ulnar nerve most commonly injured with medial pin placement
– Median nerve and anterior interosseous nerve injuries can occur from the initial trauma
Vascular Insufficiency:
– Prevalence: 5-17% at presentation
– Initial management: Rapid closed reduction and pinning without arteriography
– “White hand” (pulseless, pale hand): Emergency closed reduction required
– “Pink pulseless hand”: Management remains controversial
– Persistent vascular insufficiency after reduction: Exploration and vascular reconstruction indicated
Pin Site Infection
Pin site infections are the most common major complication of operative treatment. Closed reduction shows fewer pin site infections compared to open reduction.
Loss of Reduction
Clinical and radiological follow-up should occur at 3 weeks post-fixation to rule out loss of reduction. Early revision surgery is beneficial if loss of reduction occurs.
Cubitus Varus (Cosmetic Deformity)
Cubitus varus is a late complication resulting from malunion. Operative treatment with pin fixation has been shown to reduce the incidence of cubitus varus compared to nonoperative management.
Compartment Syndrome
Compartment syndrome is rare (~1% of cases) but represents the most devastating complication. Maintain high index of suspicion, particularly in Type III fractures and those with concomitant forearm injuries.
Follow-Up Care
– Initial follow-up: Within 1 week of treatment
– Radiographic assessment: At 3 weeks to evaluate for loss of reduction
– Pin removal: 3-6 weeks post-surgery
– Final assessment: 6 months post-injury with bilateral radiographs
– Physical therapy: Generally not necessary; most children regain full range of motion spontaneously
Prognosis
Overall functional outcomes are good for both operative and nonoperative management when appropriate treatment is selected. Functional outcomes including carrying angle, Baumann angle, elbow range of motion, and patient satisfaction are similar between operative and nonoperative treatment groups for appropriately selected Type II fractures. The number needed to treat with operative management to prevent one case of cubitus varus is 20.
Key Considerations
– All patients with suspected supracondylar fractures should be evaluated by an orthopedic surgeon
– Maintain low threshold for suspecting concomitant nerve injuries, vascular injuries, and ipsilateral distal radius fractures
– Radiographic evidence including “posterior fat pad sign” warrants orthopedic evaluation
– Type II fractures represent a heterogeneous group requiring individualized treatment decisions
– Close monitoring is essential for nonoperatively managed fractures to detect early loss of reduction
Why Choose Dr. Chambers for Hand and Elbow Care
At Raleigh Orthopaedic Clinic, Dr. Stephen Chambers specializes in hand and upper extremity surgery. With years of expertise in treating hand and elbow injuries, including Supracondylar Humerus Fracture InjuryTreatment. Dr. Chambers provides comprehensive care—ranging from at home treatments and injections to advanced hand surgery when needed. Patients trust Dr. Chambers and his team for personalized care, effective treatment options, and excellent outcomes and describe Dr. Chambers as a caring, attentive, and skilled surgeon with excellent bedside manner. His amazing team ensures every patient feels supported and informed throughout the process.
If you are experiencing wrist pain, swelling, or difficulty with wrist movements, don’t wait for symptoms to worsen. Schedule an Appointment with Dr. Chambers today to Supracondylar Humerus Fracture Treatment.and get back to normal use of your hand . Experience the benefit of specialized hand care close to home at Raleigh Orthopaedics in Raleigh, Cary, Holly Springs, and Wake Forest, North Carolina.

