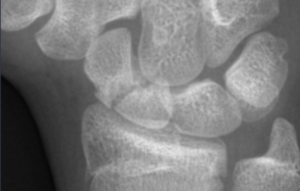
Scaphoid Fracture Treatment in Raleigh, NC
Fell and have wrist pain that won't go away? A scaphoid fracture — the sneaky wrist fracture that often looks normal on initial X-rays — is the most commonly missed wrist injury. Left untreated, it can progress to avascular necrosis and severe wrist arthritis.
What Is Scaphoid Fracture?
The scaphoid is a small boat-shaped bone in the wrist that links the forearm to the hand. It is the most commonly fractured carpal bone, typically from a fall on an outstretched hand. The challenge: up to 20% of scaphoid fractures are not visible on initial X-rays, leading to missed diagnosis when patients are told they "just sprained" their wrist.
The scaphoid has a poor blood supply — blood enters from the distal (thumb) end, meaning proximal pole fractures have high avascular necrosis (bone death) risk. Untreated or inadequately treated scaphoid fractures can progress to non-union and SNAC (scaphoid non-union advanced collapse) — a predictable pattern of wrist arthritis.
ⓘ The anatomic snuffbox test: tenderness in the hollow at the base of the thumb (with wrist extended) after a fall should be treated as a scaphoid fracture until proven otherwise — even if the X-ray looks normal. MRI is the diagnostic gold standard.
Risk Factors
Several factors increase the likelihood of developing this condition.
Fall on Outstretched Hand
FOOSH — the classic mechanism
Men 15–30
Most common demographic — peak athletic age
Snowboarding
Very common wrist fracture in boarders
Contact Sports
Blocking and falling injuries
Soccer / Football
Goalkeeper and blocking injuries
High-Energy Activities
Cycling, skateboarding, gymnastics
Stages of Scaphoid Fracture
Well-aligned fracture. Cast immobilization achieves excellent healing.
Displaced or athlete seeking faster return — surgery preferred.
Poor blood supply — high AVN risk. Non-union = bone won't heal without surgery.
Diagnosis
Initial X-rays may be normal. If clinical suspicion is high (anatomic snuffbox tenderness after fall), Dr. Chambers orders an MRI — the most sensitive test, detecting fractures within 24 hours of injury. CT scan maps fracture displacement for surgical planning.
- ✓Anatomic snuffbox tenderness
- ✓Scaphoid compression test
- ✓X-rays (PA in ulnar deviation, lateral, oblique)
- ✓MRI if X-rays normal but clinical suspicion high
- ✓CT scan for displacement assessment and surgical planning
Treatment Outcomes & Statistics
Published outcome data to help you make an informed decision.
Well-aligned waist fractures heal reliably with 8–12 weeks of casting
Longer than most fractures due to poor blood supply
Much lower union rate for proximal pole fractures — surgery preferred
Risk of non-union if fracture missed or inadequately treated
Complication Profile
| Complication | Rate | Severity | Notes |
|---|---|---|---|
| Non-union | 10–15% if missed | Serious | Leads to SNAC wrist arthritis — requires complex reconstruction |
| AVN (proximal pole) | Up to 40% | Serious | Bone death — requires vascularized bone graft |
| Stiffness after cast | Common | Minor | Hand therapy helps — most recover full motion |
| Missed diagnosis | 20% on X-ray | Serious | Always get MRI if anatomic snuffbox tender after fall |
Source: Dias et al., J Hand Surg 2008; Clementson et al., JBJS 2020
Headless compression screw fixation — excellent healing rate
Athletes return to most sports 6–8 weeks after screw fixation
Bone grafting for established non-union — good outcomes
Headless screws rarely cause problems
Complication Profile
| Complication | Rate | Severity | Notes |
|---|---|---|---|
| Screw malpositioning | 2–3% | Moderate | Addressed with revision if causing symptoms |
| AVN despite fixation | 5–10% proximal pole | Serious | Higher risk in proximal pole fractures |
| Infection | <1% | Minor | Very rare |
| Persistent non-union | 5–10% non-unions | Moderate | Additional bone graft or different reconstruction |
Source: McQueen et al., JBJS 2008; Merrell et al., J Hand Surg 2002
Treatment Options
Dr. Chambers will recommend the best approach based on your severity, goals, and lifestyle.
Thumb Spica Cast
Well-aligned distal pole and stable waist fractures can heal in a thumb spica cast over 8–12 weeks. Requires serial X-rays and CT scan at 6 weeks to confirm healing. Longer immobilization than most fractures due to poor blood supply.
Headless Compression Screw
A small titanium screw compresses the fracture ends together, achieving rigid fixation and dramatically faster healing. Athletes can return to sport in 6–8 weeks vs. 3 months with casting. Percutaneous technique (no large incision) available for acute fractures.
Bone Grafting (Non-Union)
Established non-unions require bone graft — either conventional iliac crest graft or vascularized bone graft (from the radius) to restore blood supply to the proximal fragment. Complex but effective surgery for a difficult problem.
What to Expect During Recovery
Immobilization / Post-Op
Cast or post-surgical splint. Fingers kept moving. No wrist loading.
CT Scan Confirmation
CT scan confirms fracture healing. Cast removed if healed. Begin range-of-motion exercises.
Strengthening
Progressive wrist strengthening. Return to most daily activities. Athletes begin sport-specific training.
Full Return
Full return to sport and manual work. Grip strength restored. Final CT confirms complete healing.
Frequently Asked Questions
Yes — up to 20% of scaphoid fractures are not visible on initial X-rays. If you have anatomic snuffbox tenderness (the hollow at the thumb base) after a fall, Dr. Chambers will order an MRI which detects scaphoid fractures within 24 hours of injury with near-100% sensitivity. Do not accept "just a sprain" if your wrist pain persists beyond 2 weeks.
Undisplaced distal fractures occasionally heal spontaneously, but this is unpredictable and risky. Proximal pole and displaced fractures almost never heal without treatment. Untreated fractures progress to non-union, avascular necrosis, and SNAC wrist arthritis — a serious, often irreversible condition. Always get proper diagnosis and treatment.
8–12 weeks for cast treatment — significantly longer than most fractures because of the scaphoid's poor blood supply. This is one reason many active patients and athletes choose surgical fixation, which achieves union in 6–8 weeks with early motion.
SNAC (Scaphoid Non-Union Advanced Collapse) is a predictable pattern of wrist arthritis that develops when a scaphoid non-union is left untreated for years. The wrist collapses in a characteristic pattern causing significant pain and loss of motion. This is why early diagnosis and treatment of scaphoid fractures is so important.
Related Conditions & Resources
Wrist Pain After a Fall? Get an MRI — Not Just an X-ray.
Scaphoid fractures are commonly missed. Same-week appointments available. No referral needed.

Stephen Chambers, M.D.
Dual Board-Certified Hand & Upper Extremity Surgeon · Raleigh Orthopaedic










